Osteoarthritis (OA)
Let’s first talk about osteoarthritis (OA). OA is the arthritis commonly associated with older age and “wear and tear” on the joints. As we get older and use our bodies, we can develop OA, which is irritation within the joint resulting from breakdown of the cartilage. Cartilage is meant to cushion and protect the joint, and when it breaks down it can result in pain and inflammation. OA can happen anywhere in the body but is commonly seen in the knees, hips, and even in the spine. OA can happen bilaterally (meaning on both sides of the body) or unilaterally (just on one side) depending on use of the joints. For example, if somebody’s job requires them to kneel and they repeatedly favor one leg to get up and down, that knee may develop OA sooner than the other. Other factors, such as prior injuries to a joint, can put that joint at higher risk of developing OA. OA is typically diagnosed with an x-ray and can be managed by an orthopedic specialist.
Rheumatoid Arthritis (RA)
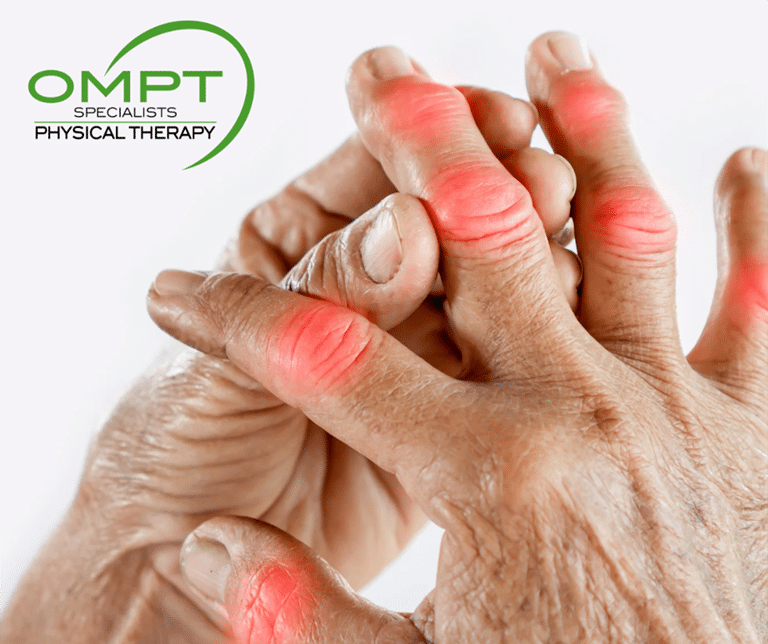
Now let’s talk about rheumatoid arthritis (RA). RA is actually an autoimmune disease, meaning the body’s own immune system will attack its joints and cause inflammation resulting in breakdown and pain. RA is typically bilateral (for example, somebody could have symptoms in both of their hands opposed to just one). Symptoms commonly include pain, visible swelling, and even redness at the joints. It commonly affects smaller joints like in the hands or feet, but can also affect larger joints like the elbows, knees, or hips. A lot of people will experience worse symptoms earlier in the morning within the first hour of waking up. It is common for people with RA to experience episodes of exacerbations (flare ups) and episodes of remission (minimal or no symptoms). Symptoms can become flared up by a number of factors including stress, medication changes, or illness because of a weakened immune system. RA will be diagnosed with multiple tests including imaging (like x-rays) and blood tests. Because it is an autoimmune disease, it will typically be diagnosed and managed by a rheumatologist.
Arthritis management
While there is no cure for either type of arthritis, management can include several strategies, including physical therapy. Physical therapists have a wide variety of treatment techniques that can manage pain/swelling and improve strength and mobility in and around the joint to reduce symptoms and slow the progression of the arthritis. Different types of arthritis will likely be managed differently, and treatment can look different for everyone. While arthritis is extremely common and there is no true “cure,” that does not mean people have to live with symptoms every day for the rest of their lives. If you have been diagnosed with or suspect you may have any type of arthritis, come experience the OMPT difference and learn some individualized management strategies from one of our knowledgeable physical therapists!